Healthremedy123.com – The Thoracic Spinal Fusion procedure can change the shape and function of your spine. It can cause an uneven distribution of stress throughout your spine, which accelerates wear and tear on vertebral joints. Luckily, there are some proven benefits to this procedure. Let’s look at some of them. After reading this article, you’ll be ready to make a decision based on the information you’ve gathered.
Higher Risk of Recurrent Disc Herniation
Compared to the non-operative control group, the non-union control group had higher initial and final outcome rates. However, there was no difference in percent recovery at 1-year follow-up. The patients in the non-union group also had a higher risk for degenerative joint disease, and their outcomes were not better. Despite these benefits, there are also a number of risks with this procedure. There are several potential complications of this surgery, including a higher risk of a recurrent herniated disk, an increased rate of disc degeneration, and an increased incidence of pain and complication in the non-union group.
Minimally invasive spine surgery is not for everyone. If your spine is unstable, minimally invasive surgery may be the right option. In unstable patients, the surgery will decompress the spine’s levels and stabilize it with solid fusion. The technique used for each patient will depend on the particular problem. In some cases, decompression laminoplasty alone will be performed. For those who are worried about undergoing the surgery, you can discuss the pros and cons with your surgeon.

The procedure itself is not very complicated and will take three to four hours. Patients are usually released after three or four days. Pain medications may be prescribed. Post-operative recovery depends on the patient’s bone healing ability and the location of the incisions. After spinal fusion, you’ll likely need to wear a brace. You may also require internal fixation using screws and plates. Infection is a risk, so antibiotics may be prescribed.
Spinal Fusion Procedure Corrects Deformities
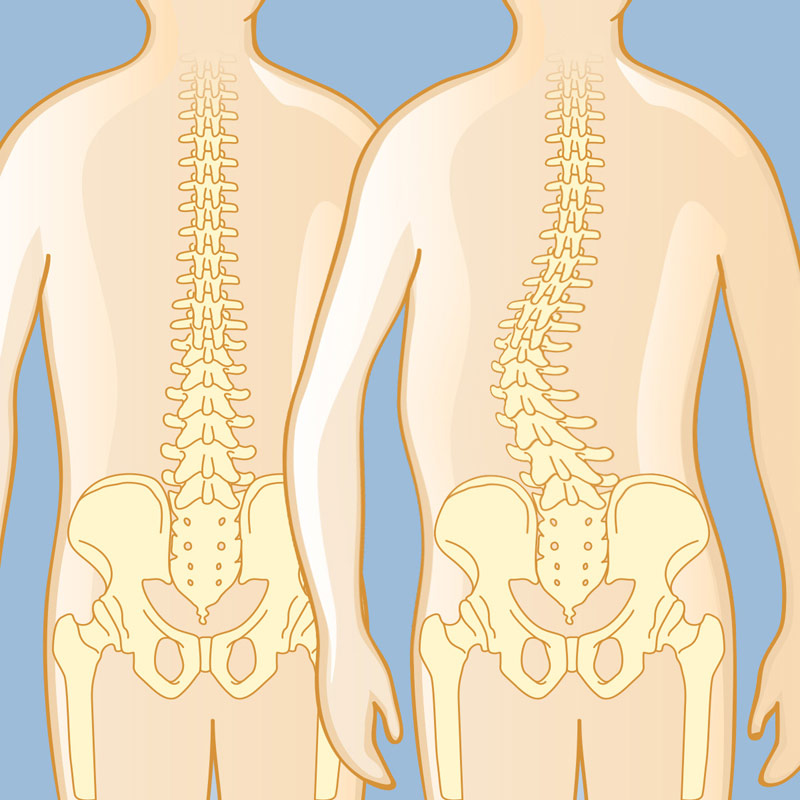
Aside from preventing degenerative disease, a spinal fusion procedure can also correct deformities. A common problem, spondylolisthesis, is when one vertebra slips forward onto the vertebra below it. If the fusion is not done correctly, it can lead to pressure on the nerve, which could result in numbness or pain in the extremity served by the affected vertebra.
Researchers have conducted several trials examining the benefits and risks of fusion. One study compared the effectiveness of fusion with nonsurgical therapy and interdisciplinary rehabilitation. Overall, fusion had a high success rate (67%) but a low failure rate. Another study concluded that the procedure had little or no benefit for nonsurgical treatments. In addition, a randomized trial of fusion was not performed in enough cases to show that it is a viable treatment option.
As with any surgery, the Thoracic Spinal Fusion procedure should be performed only by a board-certified neurosurgeon or orthopedic surgeon with complex training in spinal fusion. Inadequate training can lead to a failed spinal fusion. A highly experienced surgeon can safely perform the procedure while protecting the integrity of the nervous system. The patient is in good hands when undergoing spinal fusion, so it’s vital to make the right decision regarding your doctor.
History of Spine Deformities
The outcome of the procedure is determined by the patient’s condition. The risks of a successful surgery are the same for patients who have a traumatic injury or who have a history of spinal deformity. The risks of a successful surgery depend on the individual’s age, the type of tumor, and the surgical levels. The study authors concluded that LAMP is a safe option for some patients, but the lack of adequate data and high-quality RCT studies undermine its validity.
During the recovery period, most patients will spend one to two nights in the intensive care unit. An epidural anesthetic is administered to ensure that the patient experiences virtually no pain during the first 24 hours after surgery. Patients are then mobilized in a lumbar brace with a physiotherapist. Most patients are happy to complete their procedure. If a patient experiences a significant degree of pain after surgery, he or she should seek immediate medical care.
Surgical interventions are often not the best option for patients with chronic back pain. In some cases, the procedure may not be necessary, but it will only improve the condition of the patient. Patients should consider nonpharmacologic treatment for their condition before undergoing this procedure. These options may include spinal manipulation, intensive inter-disciplinary rehabilitation, yoga, and cognitive-behavioral therapy. In addition to these options, fusion is considered a reasonable option for chronic back pain patients. We really appreciate and welcome guest post submissions from you.
Reference:


